A pregnancy test, as the name implies, is simply a test used to determine whether or not a woman is pregnant. Often used early in the form of a home pregnancy test, this process is helpful in making an early determination. An unborn child will require medical care even before they arrive and an early diagnosis is important so that the mom-to-be can learn the best types of food to consume, begin pregnancy classes and prepare for the family’s new addition.
The most popular type of pregnancy test, which is used for early detection, is a home pregnancy test. These can be found at most major retail and/or drug stores and can provide quick results. Because these are amateur tests, meaning they are not performed by a licensed medical doctor, there is always the possibility of a false reading.
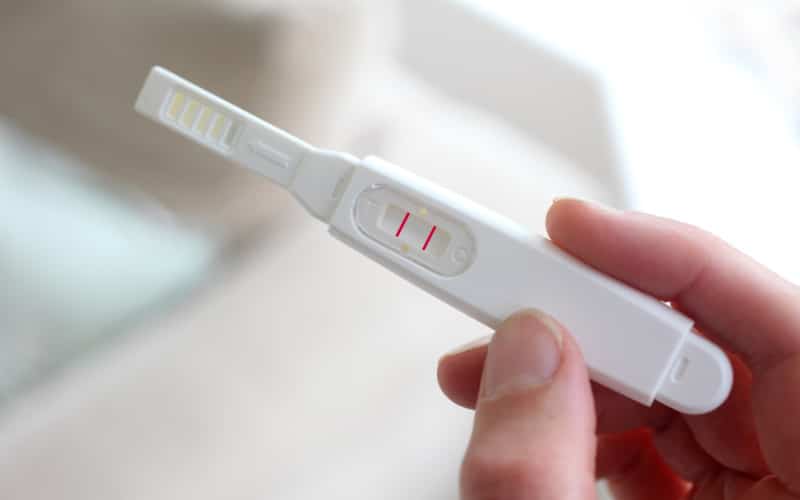
If the directions are followed correctly, however, the accuracy rate is quite respectable. Before seeing a doctor, many women want to have an idea as to whether or not they are pregnant, which is why an at home pregnancy test is very popular.
Depending on the results of a home pregnancy test, a woman may still wish to consult a physician to ensure certainty. During the visit, a physician will relay the determination of pregnancy or the absence thereof and, if necessary, will provide additional information for expectant moms.
It can be difficult to realize the symptoms of pregnancy for first-time moms-to-be, which is why it is important to learn about the possible signs of an early pregnancy. Among them, an increased sensitivity to certain foods and/or smells, recurring morning sickness, fatigue, exhaustion and mood swings.
It is important to have a pregnancy test following the onset of any or all of these symptoms because a positive result means that a new change in lifestyle may be in order. Pregnant women will likely be instructed to avoid air travel, smoking or being near secondhand smoke and the consumption of alcohol.
Any and all of these can be harmful to a child and should therefore be avoided. It is very important that pregnant women speak with their doctor about the best ways to ensure the development of a healthy child.
This article is to be used for informational purposes only. It is not designed to be used in place of, or in conjunction with, professional medical advice and/or recommendations. A woman who believes that she may be pregnant should consult a licensed medical doctor for a pregnancy test and the best method of ensuring the health of her unborn child.
Did you like this? Help us reach more people sharing it on social networks. Thanks!





 Prematurity is the most common cause of sickness and death among newborns. Babies born before the 37th week of pregnancy are often called preterm or “premature”, babies born before the 32nd week are considered very premature, babies born before the 28th week are considered extremely premature. Generally, babies born after the 25th week of pregnancy have a survival rate of between 50-60% (although they will stay an extended period of time in intensive care), which increases dramatically to over 90% after the 28th week.
Prematurity is the most common cause of sickness and death among newborns. Babies born before the 37th week of pregnancy are often called preterm or “premature”, babies born before the 32nd week are considered very premature, babies born before the 28th week are considered extremely premature. Generally, babies born after the 25th week of pregnancy have a survival rate of between 50-60% (although they will stay an extended period of time in intensive care), which increases dramatically to over 90% after the 28th week.