 In pregnancy, your skin may begin to change right before your eyes. These changes are a very common and usually an expected part of pregnancy, although not every woman will experience all the same skin changes. Most skin changes during pregnancy can be blamed on the effects of various hormones. These ever-fluctuating pregnancy hormones can do some strange things to your skin, but most changes are not permanent and they tend to disappear within a few months after you give birth, although they generally come back in subsequent pregnancies. Except for affecting your appearance cosmetically, most common skin changes don’t harm you or your unborn baby in any way.
In pregnancy, your skin may begin to change right before your eyes. These changes are a very common and usually an expected part of pregnancy, although not every woman will experience all the same skin changes. Most skin changes during pregnancy can be blamed on the effects of various hormones. These ever-fluctuating pregnancy hormones can do some strange things to your skin, but most changes are not permanent and they tend to disappear within a few months after you give birth, although they generally come back in subsequent pregnancies. Except for affecting your appearance cosmetically, most common skin changes don’t harm you or your unborn baby in any way.
Pregnancy Stretch Marks
Stretch marks. We’ve all heard of them and we’ve all hoped they wouldn’t strike us during pregnancy, but the fact is 50- 90% of pregnant women are affected by them to some extent. Most appear on the abdomen, breasts, hips and thighs during the second and third trimesters. Keep your weight gain within the recommended range, apply a nourishing lotion to your stretching skin daily to keep it well moisturized and eat a sensible, well-balanced diet, as well as drink plenty of water to help keep your skin as healthy as possible.
Pregnancy Glow
One of the few desirable changes that may occur to your skin during pregnancy is often called, “the glow of pregnancy”. Friends and family (and complete strangers) may comment on it, while you may not even notice the difference. Hormonal changes and increased blood circulation tend to make your oil glands work overtime, causing your face to appear shinier than normal, as well as make your cheeks look rosier.
Skin and Hormones
There are a few less desirable skin changes you can expect during pregnancy. Hormonal changes are also responsible for the unwelcome and very aggravating change of pimple outbreaks (those oil glands working overtime). However, depending on your hormones and skin condition, you may not suffer from this problem at all. Occasionally, long-term acne conditions may actually clear up during pregnancy, if you are lucky. If you become bothered with acne breakouts, keep a strict cleansing routine, by washing your face twice a day (more often can lead to dry skin) with a mild over-the-counter cleanser. Stay away from medicated acne creams or scrubs, without checking with your doctor or midwife first, because some may contain substances that are not recommended for pregnant women.
Skin Itching in Pregnancy
Itchiness and dryness is a common problem during pregnancy, particularly in relation to your growing belly and breasts. The skin across your abdomen may become very itchy as it stretches and tightens, as well as your breasts as they enlarge. You may also find that your palms and/or soles are red and itchy, which is likely caused from higher estrogen levels. Try to avoid scratching, which may only aggravate the problem and make it worse. Instead, moisturize with lotion and avoid hot showers and baths (which you should already be avoiding during pregnancy). A warm oatmeal bath may help alleviate some of discomfort, if it becomes unbearable. You can buy pre-mixed oatmeal bath preparations at many drugstores. If you have bothersome itching that doesn’t go away or becomes worse, contact your doctor or midwife to make sure there’s not an underlying medical problem causing your symptoms.
Rashes
Sometimes during the last 1-2 months of pregnancy, women experience red, itchy, pimply skin eruptions. This is a common skin condition called “pruritic urticarial papules and plaques of pregnancy” or PUPPP for short, which occurs in about one in every 150 pregnancies. It usually begins on the abdomen and spreads to the thighs, upper arms and sometimes the buttocks, but thankfully never the face. PUPPP is not harmful to you or your baby and will disappear after you give birth, although it can reappear in subsequent pregnancies, though it generally only appears during first pregnancies. Your doctor or midwife will most likely prescribe a topical anti-itch ointment or possibly an oral medication to help alleviate the intense itchiness.
Pregnancy Mask
Sometimes during the second trimester of pregnancy, women develop chloasma or “the mask of pregnancy”. Chloasma generally appears as irregular brown patches on your face. They are most common on the forehead, cheekbones, nose and chin, as a result of increased pigmentation caused by those wonderful pregnancy hormones at work once again. The good news is: they gradually will fade after delivery. There”s not a whole lot you can do to prevent Chloasma, but wearing a good sunscreen and avoiding direct sunlight can help keep your skin from producing even darker pigmentation. Concealing makeup applied to your face can help even out facial tones. If any changes in skin pigmentation are accompanied by pain, tenderness or redness or if you notice any changes in the color or size of a mole, don’t hesitate to let your doctor or midwife know immediately.
Linea Nigra
During the last half of pregnancy, you may notice a dark line running down the middle of your belly from the top to the bottom. This is common and is called the “linea nigra”. This line is normally there, but those wacky pregnancy hormones tend to darken this line, making it more noticeable. Thankfully, it will fade back to normal after delivery.
 Pregnancy is one of the most difficult and stressful experiences a teen might ever face. If you are a teen facing an unplanned pregnancy, you are not alone. Millions of other teens have gone through (and survived!) the same thing and most of those pregnancies were unplanned also. You may have been surprised when you found out or even hoped it wasn’t true. One of the first thoughts that may come to mind is that your life is over, fortunately, that isn’t so. Before you freak out, take a deep breath and just remember you are in charge of your life. There are many resources available to you.
Pregnancy is one of the most difficult and stressful experiences a teen might ever face. If you are a teen facing an unplanned pregnancy, you are not alone. Millions of other teens have gone through (and survived!) the same thing and most of those pregnancies were unplanned also. You may have been surprised when you found out or even hoped it wasn’t true. One of the first thoughts that may come to mind is that your life is over, fortunately, that isn’t so. Before you freak out, take a deep breath and just remember you are in charge of your life. There are many resources available to you.



 If you’re going through pregnancy, you may be wondering if it’s safe for you to travel & also what extra precautions you should take during your time away. If you are in good health and you’ve already spoken with your doctor or midwife about possible risks and potential problems that may arise (especially if planning to travel abroad), the decision is all yours. Pregnancy travel — this may be the last time you’ll have a chance to get away with your partner for a while; just the two of you.
If you’re going through pregnancy, you may be wondering if it’s safe for you to travel & also what extra precautions you should take during your time away. If you are in good health and you’ve already spoken with your doctor or midwife about possible risks and potential problems that may arise (especially if planning to travel abroad), the decision is all yours. Pregnancy travel — this may be the last time you’ll have a chance to get away with your partner for a while; just the two of you.


 In pregnancy, your skin may begin to change right before your eyes. These changes are a very common and usually an expected part of pregnancy, although not every woman will experience all the same skin changes. Most skin changes during pregnancy can be blamed on the effects of various hormones. These ever-fluctuating pregnancy hormones can do some strange things to your skin, but most changes are not permanent and they tend to disappear within a few months after you give birth, although they generally come back in subsequent pregnancies. Except for affecting your appearance cosmetically, most common skin changes don’t harm you or your unborn baby in any way.
In pregnancy, your skin may begin to change right before your eyes. These changes are a very common and usually an expected part of pregnancy, although not every woman will experience all the same skin changes. Most skin changes during pregnancy can be blamed on the effects of various hormones. These ever-fluctuating pregnancy hormones can do some strange things to your skin, but most changes are not permanent and they tend to disappear within a few months after you give birth, although they generally come back in subsequent pregnancies. Except for affecting your appearance cosmetically, most common skin changes don’t harm you or your unborn baby in any way.










 If you are pregnant, you may be wondering if tanning during pregnancy is safe for your unborn baby. You may dread the thought of looking pale especially if you are used to seeing a sun glow when you look in the mirror.
If you are pregnant, you may be wondering if tanning during pregnancy is safe for your unborn baby. You may dread the thought of looking pale especially if you are used to seeing a sun glow when you look in the mirror.

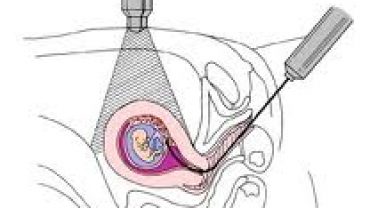
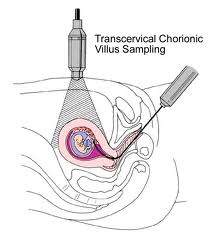 Chorionic villus sampling is usually done early in pregnancy between the 9th and 13th week. This is a procedure that involves removing a sample of chorionic villi cells from the placenta at the point where it attaches to the uterine wall.
Chorionic villus sampling is usually done early in pregnancy between the 9th and 13th week. This is a procedure that involves removing a sample of chorionic villi cells from the placenta at the point where it attaches to the uterine wall.